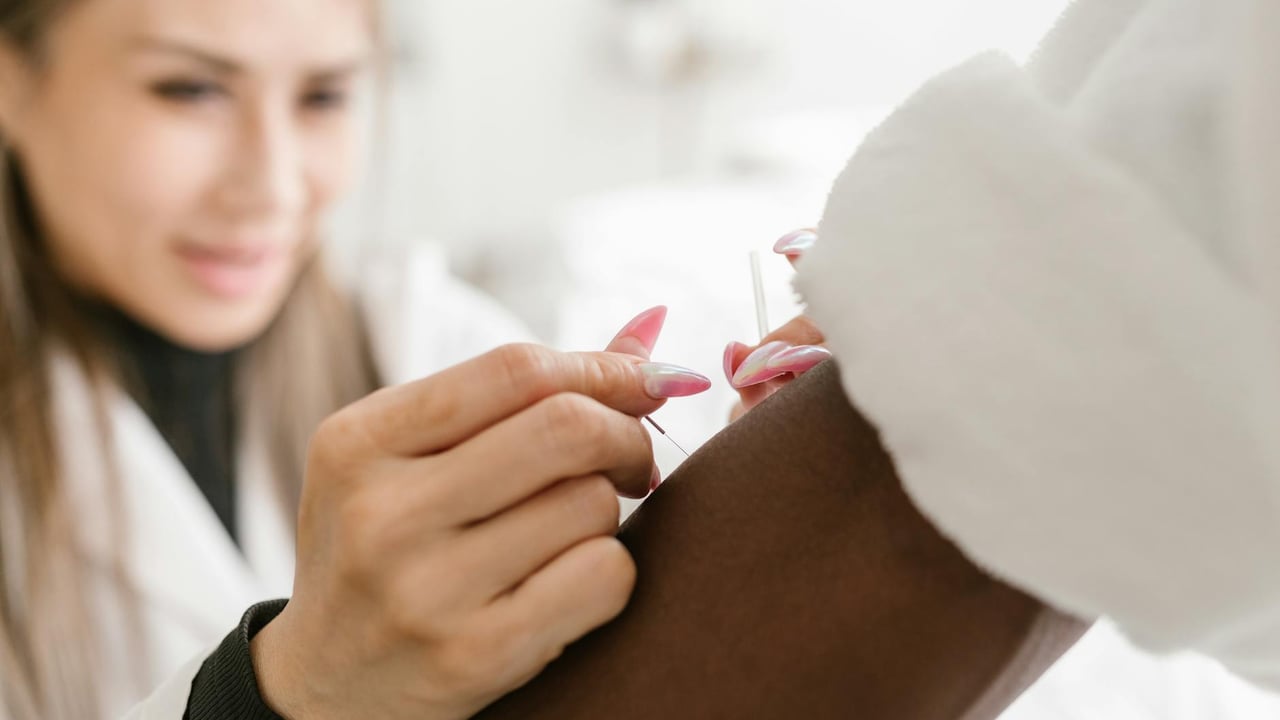
On a chilly March morning at the PLA General Hospital, patients queue silently outside the acupuncture clinic run by Chief Physician Guan Ling. She speaks softly to first-timers, steadies a trembling hand and inserts a silver needle with the practiced economy of someone who has spent decades turning an ancient therapy into a pragmatic tool for soldiers. The scenes are intimate, quotidian and carefully staged: a nervous woman whose sudden deafness improves after treatment, a sailor relieved of chronic tinnitus, a soldier on a training ground who finds immediate ease from acute knee pain.
Guan’s trajectory reads like a personal and institutional arc: from literature-leaning schoolgirl to a top herbal- and needle‑wielding clinician at one of China’s premier military hospitals. Trained under the noted Shanxi acupuncturist Xie Xiliang, she was admitted to the PLA General Hospital after years of study and then set about professionalising a small acupuncture ward that once struggled for credibility. Over time she married classical acupuncture with modern anatomy and rehabilitation science to develop what she calls “structural acupuncture,” an approach that targets tense muscle and fascial chains with targeted needling and manual techniques.
The practical impetus was simple: soldiers were returning from repetitive, high‑impact training with stubborn musculoskeletal injuries that undermined unit readiness. Guan began experimenting with anatomy texts and English literature, translating dense technical passages herself and reconciling them with meridian theory. The result, she says, is a technique that locates and relaxes specific myofascial structures, often achieving faster functional relief than traditional local needling alone.
Guan’s clinic now reports impressive outreach. The acupuncture unit says it has provided more than 300,000 consultations and trained over 100,000 frontline medical staff and soldiers in basic non‑pharmaceutical self‑care. A rolling training programme has reached roughly 130,000 service members, taught nearly 10,000 medics cupping techniques and trained almost 1,000 military physicians in acupuncture. In a 2025 pilot called “No‑Knee‑Pain Barracks,” organisers report a 70% fall in training‑related knee pain and an 80% reduction in drug use among participating units.
Those figures, promoted in state media, point to a broader institutional objective: low‑cost, scalable methods to protect troop health and conserve medical resources. Guan’s team stresses frugality and portability — lessons drawn from repeated deployments to deserts, highlands and naval vessels — and prides itself on techniques that allow many minor injuries to be treated on site so soldiers can continue training. Field vignettes in official accounts underline an ethic of proximity: the clinician who squats beside a wounded soldier on a tyre, the physician who stays through the coldest night to ensure a unit gets through allergy season.
The institutional context is significant. The People’s Liberation Army has been investing in integrated medicine as part of broader efforts to modernise force health protection without ballooning budgets. Traditional Chinese medicine (TCM) enjoys political support in Beijing and is being incorporated into military medical doctrine where it suits readiness and logistical constraints. Acupuncture’s portability and low material cost make it an attractive adjunct to conventional care, especially in austere environments where pharmaceuticals and imaging are scarce.
Yet the expansion of acupuncture in military settings raises questions for outside observers. The international medical community generally asks for controlled trials and reproducible outcomes; state media case studies, vivid though they are, do not substitute for randomized evidence. There is also a reputational tension: proponents present structural acupuncture as a synthesis of modern anatomy and Chinese tradition, while sceptics worry about overclaiming benefits and underreporting adverse events. For the PLA, however, the metric is operational utility rather than academic consensus.
Guan’s professional story also carries geopolitical resonance. Medical practices that improve troop endurance have internal security value, and successful, exportable low‑cost therapies bolster China’s soft power narrative. Demonstrated gains in reducing drug use and preserving combat strength could be leveraged in defence diplomacy and training exchanges, particularly with partners that prize low‑resource medical solutions.
If the anecdotal and pilot data hold up under independent scrutiny, the most tangible implication is simple: armies that keep soldiers healthy with cheap, field‑ready interventions have a durability advantage. Even if the mechanism of effect is contested, the PLA’s adoption of a standardised acupuncture curriculum and its rapid dissemination through the force show how medical policy can be as much about logistics and culture as about clinical science. For now, Guan Ling’s silver needle is less a cure‑all than a symbol of how tradition, institutional backing and pragmatic adaptation can combine to reshape military medicine.